The study, funded by Providence Medical Technology, Inc., comes a year after the FDA granted clearance to market for the company’s Corus™ Spinal System for minimally invasive Posterior Cervical Fusion (PCF) specifically for cervical degenerative disc disease. The system allows more tissue sparing than a traditional open posterior approach and has potentially fewer comorbidities than anterior fusion.
Meta-analysis evaluates PCF outcomes
The study analyzed the patient-reported outcomes data from 33 previously published articles involving a total of 1238 patients treated for spondylosis, spinal stenosis and degenerative disc disorders resulting myelopathy or radiculopathy. The findings were published online May 7, 2019 ahead of print in THE SPINE JOURNAL.[1]
“Our analysis shows that posterior cervical fusion with decompression resulted in significant clinical improvement,” says co-author Morgan Lorio, MD, an investigator for the study and a member or the AOPM medical staff. “When you take into account the patient-reported outcomes along with the high fusion rates and low rates of revision and of complications and adverse events, our study validates the posterior approach as an option that may be considered in selected patients.”
While 33 studies were included in the systematic review, two were excluded from the meta-analysis due to randomization methods that could not be fully evaluated. The researchers analyzed the data for all outcomes and did two sub-group analyses, one for studies in which only myelopathy or radiculopathy (or both) were stated as surgical indications, and the other subgroup of studies evaluated only myelopathy or Ossification of the Posterior Longitudinal Ligament (OPLL), or both as surgical indications.
For clinical outcomes, the pooled rates of successful fusion were:
- 98.3 % for all indications,
- 98.9% for myelopathy/radiculopathy, and
- 97.1% for myelopathy/OPLL
For revisions:
- 1.09% for all indications,
- 0.81% for myelopathy/radiculopathy, and
- 1.41% for myelopathy/OPLL
Pooled complication rates were:
- 9.02% for all indications,
- 7.07% for myelopathy/radiculopathy
- 13.18% for myelopathy/OPLL
Four measures of patient reported outcomes used
The studies used the visual analog scale (VAS), neck disability index (NDI), Japanese Orthopedic Association (JOA) score or the modified Japanese Orthopedic Association (mJOA) score to measure patient reported outcomes.
For all indications and for both subgroup analyses, patients reported a significant improvement. The highest improvement was reported in the myelopathy/radiculopathy subgroup on the VAS, NDI, JOA and mJOA scores, which corresponded with the highest fusion rates and lowest revision and complication rates in the clinical outcomes.
The primary limitation of this study is that the majority of studies (20 of 31) were retrospective. Another limitation was that two of the studies were judged to have a high risk of bias, and while included in the review, were excluded from the meta-analysis. Nevertheless, the authors concluded that PCF with decompression be considered a surgical option in selected patients.
In a direct comparison of outcomes for anterior cervical fusion (ACF) and PCF, Yue and colleagues found that while PCF patients had a higher rate of post-operative transfusions, they had lower risk of 30-day complications. The authors suggested the higher transfusion rate for PCF may be due to increased surgical blood loss in exposing the spine via stripping of the muscle off bone, osteoporotic bone with wider vascular channels, and epidural bleeding following laminectomy.[2]
The Corus™ system uses ultra-thin (less than 1 cm) instruments to reduce dissection and stripping of muscle tissue and assists surgeons in performing the steps of a traditional Posterior Cervical Fusion.
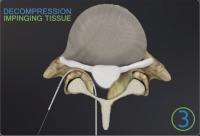
With smaller incision and decreased stripping, the system significantly reduces blood loss compared to open PCF. The posterior approach preserves access to the anterior spine for future reconstructive surgery if necessary. In addition, the approach provides indirect neural decompression without the need for directly decompressing the involved nerve root.
In a 2016 clinical trial of 10 selected patients with cervical spondylotic radiculopathy treated with the Corus™ system achieved significant symptom relief after one-year of follow up.[3]
At Advanced Orthopedics, our goal is to help you feel better and heal faster. Combined with extensive experience, innovative technology, and advanced treatments we are able to provide you the complete array of treatment options, including advanced minimally invasive surgery, to allow you to consider all the treatment options for your condition. We are happy to review your MRI and discuss your options and answer all your questions to ensure you get the best treatment for you. For more information contact us at (407) 960-1717.
[1] Youssef, Jim A, Anneliese D. Heiner, PhD, Jana R. Montgomery, PhD, Gabriel C. Tender, MD, Morgan P. Lorio, MD, FACS, Joseph M. Morreale, MD, Frank M. Phillips, MD. “Outcomes of Posterior Cervical Fusion and Decompression: A Systematic Review and Meta-analysis.” The Spine Journal. DOI: https://doi.org/10.1016/j.spinee.2019.04.019
[2] Yue, John K, Pavan S Upadhyayula, Hansen Deng, David C Sing, Joseph D Ciacci. “Risk Factors for 30-day Outcomes in Elective Anterior Versus Posterior Cervical Fusion: A Matched Cohort Analysis.” Journal of Craniovertebral Junction & Spine vol. 8,3 (2017): 222-230. DOI:10.4103/jcvjs.JCVJS_88_17
[3] Bruce M. McCormack, Edward E, John C2, Siemionow K. “Minimally Disruptive Posterior Cervical Fusion with DTRAX Cervical Cage for Single Level Radiculopathy - Results in 10 Patients at 1-Year.” Spine Research.